How does the endodontic treatment work
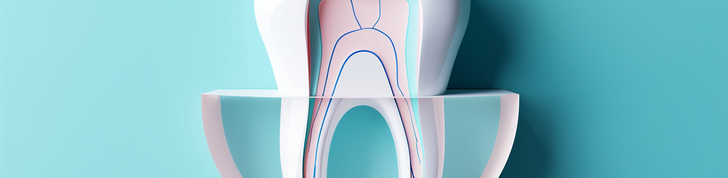
The purpose of endodontics is to preserve the tooth in the oral cavity and restore its function. To achieve this, the tooth root canal system must be properly treated. During the procedure, we mechanically widen, chemically disinfect, and fill the canals of the damaged tooth so that we can subsequently reconstruct the tooth and, if necessary, address any inflammation of the bone bed if diagnosed.
Depending on the complexity of each case, we divide the endodontic treatment into the appropriate number of visits. Each visit lasts approximately two hours. Endodontic procedures are performed under local anesthesia, or in controlled analgesia for enhanced patient comfort. The treated tooth is first isolated with a special elastic membrane (called a rubber dam). In cases of significant damage to the tooth crown, we perform adhesive reconstruction of the crown walls before isolating the tooth.
Throughout the treatment, we use special instruments and take X-rays for precise monitoring. First, we remove the infected tissue from the crown portion of the dental pulp and locate the entrances to the root canals using an operating microscope. The root canal system is then mechanically widened using manual and rotary tools, and disinfectant solutions are applied to eliminate harmful microorganisms.
The exact length of each root canal is determined using an electronic apex locator. Once the canals have been expanded and disinfected, they are filled and sealed with gutta-percha pins. In cases where the root system contains infected or inflamed tissue, a disinfectant paste with calcium hydroxide is applied initially, and the root canals are filled definitively during a subsequent visit. Finally, we complete the core buildup of the tooth crown, preparing it for any necessary prosthetic restoration.